WHAT SHOULD ONE KNOW ABOUT PSORIASIS?
Psoriasis is a chronic autoimmune skin disease that causes red, itchy scaly patches, most commonly on the knees, elbows, trunk and scalp. Psoriasis is an immune system problem that causes the skin to regenerate at faster than normal rates.
Psoriasis is a disease that runs in families. If a parent, grandparent, brother, or sister has psoriasis, there is a greater possibility of the person getting it.
What does psoriasis look like?
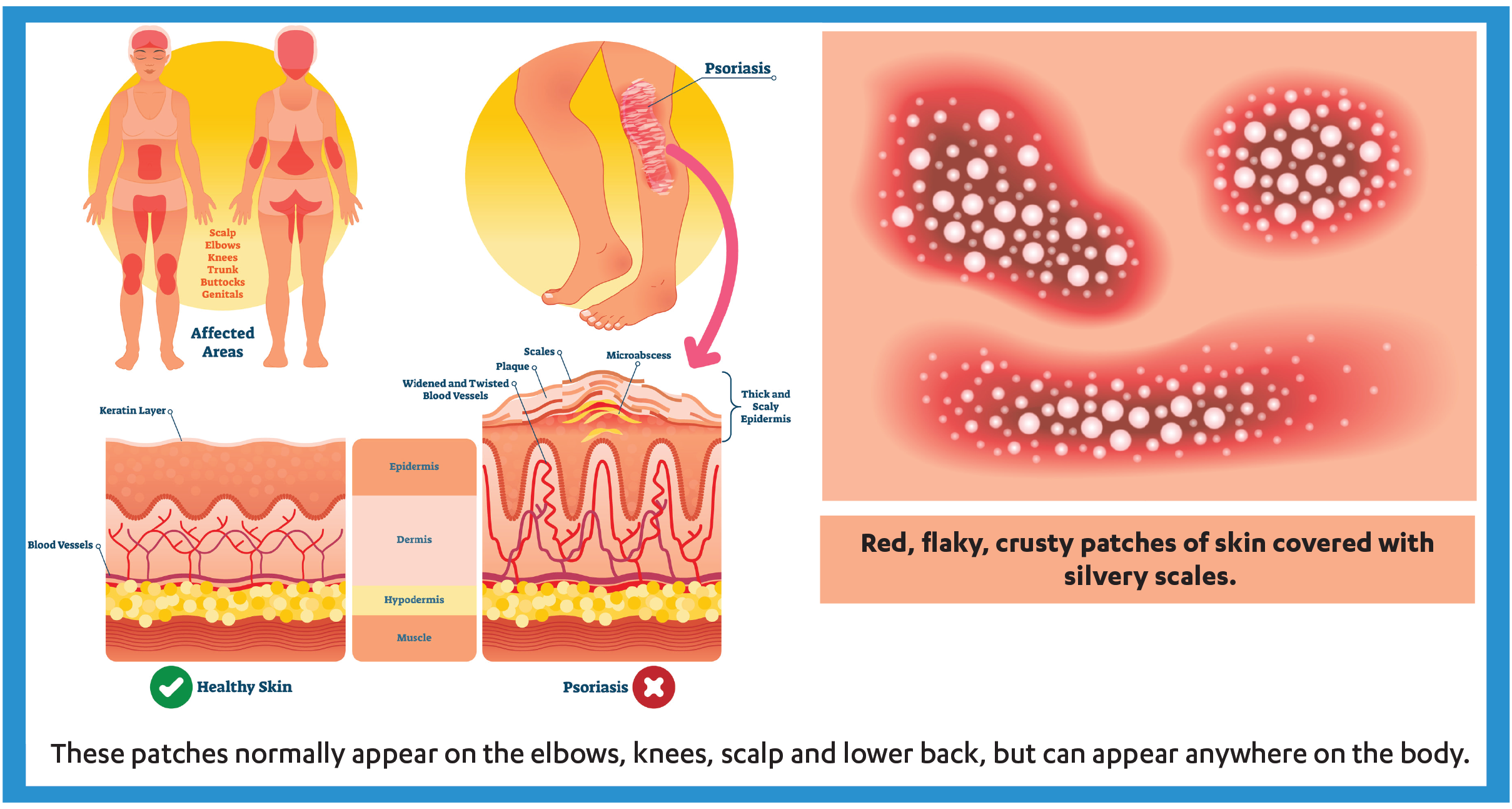
Swelling and redness around the scales are fairly common. Typical psoriatic scales are whitish-silver and develop in thick, red patches. Sometimes these patches might crack and bleed.
Scales typically develop on joints, such as elbows and knees. They may develop anywhere on the body, including the:

Hands

Feet

Neck

Scalp

Face
Plaque psoriasis
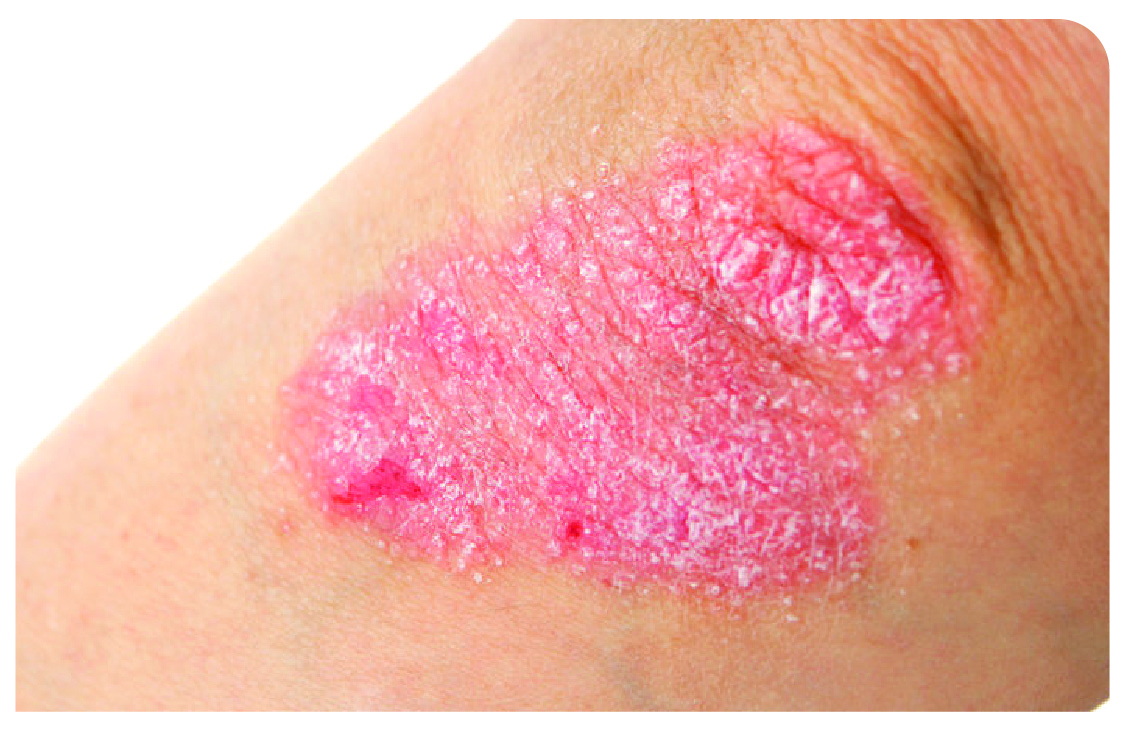
Patches of thick raised skin covered with silvery scales
Scalp psoriasis
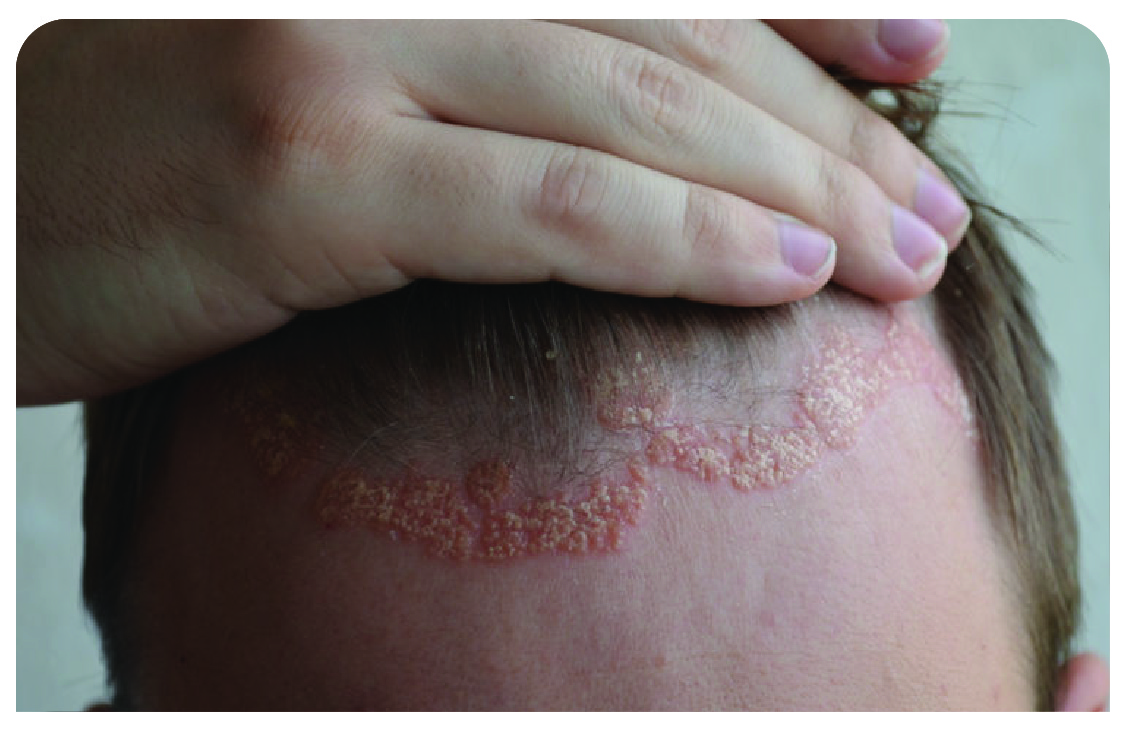
Thin or thick patches that could cause hair loss
Nail psoriasis
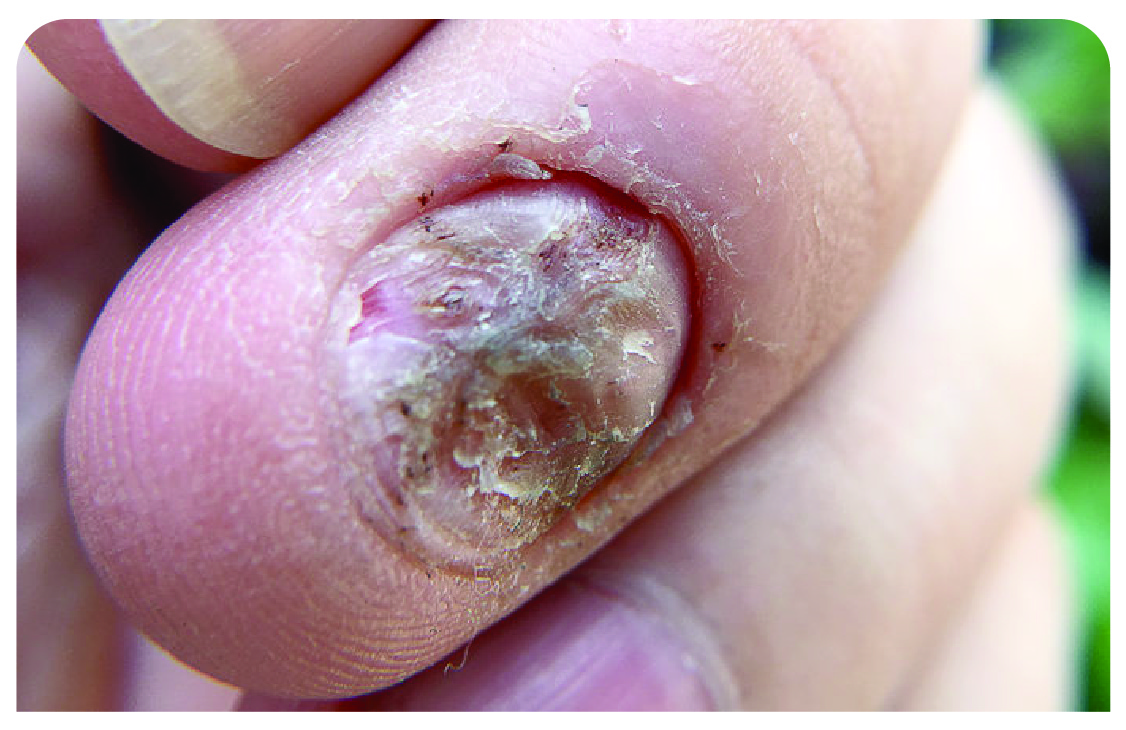
Yellow-brown spots on the nails, pitted nails, crumbling nails, and nails separating from fingers or toes
Guttate psoriasis

Common in children who have had an infection like strep throat. Could cause many small, scaly spots
Inverse psoriasis

Common in armpit and groin area. Shiny, smooth patches instead of scaly ones
Pustular psoriasis
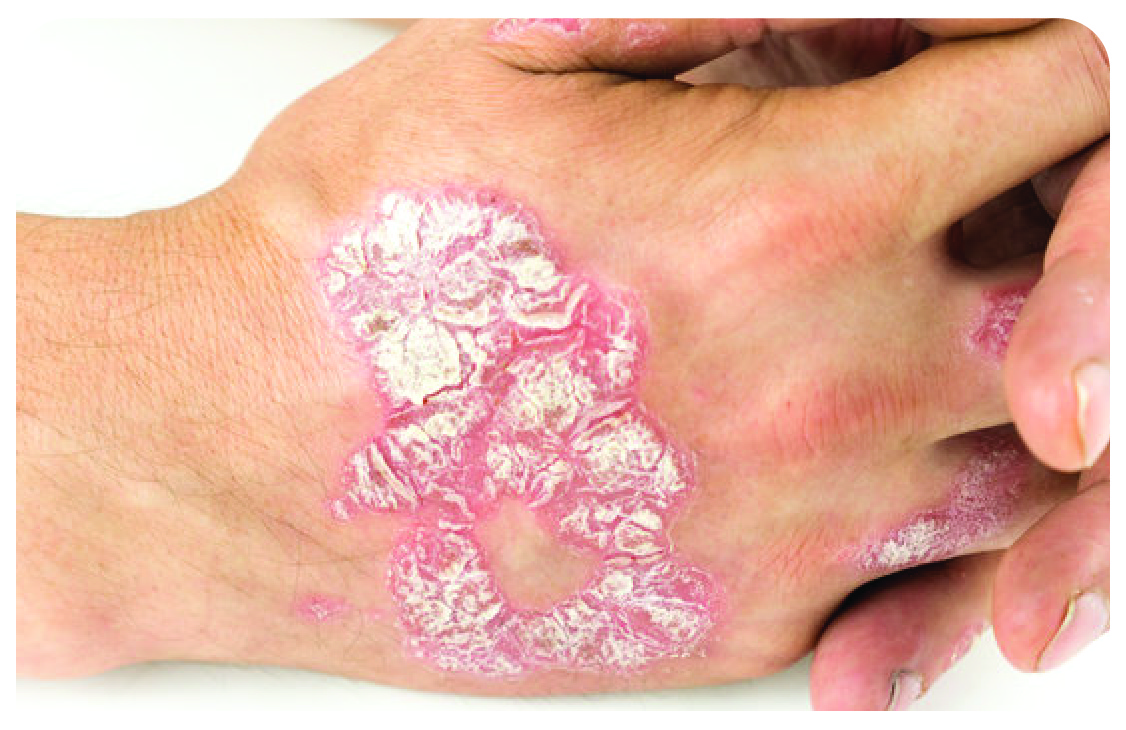
Painful pus-filled blisters and thick, scaly skin that can crack easily (on hands and feet)
Generalized pustular psoriasis
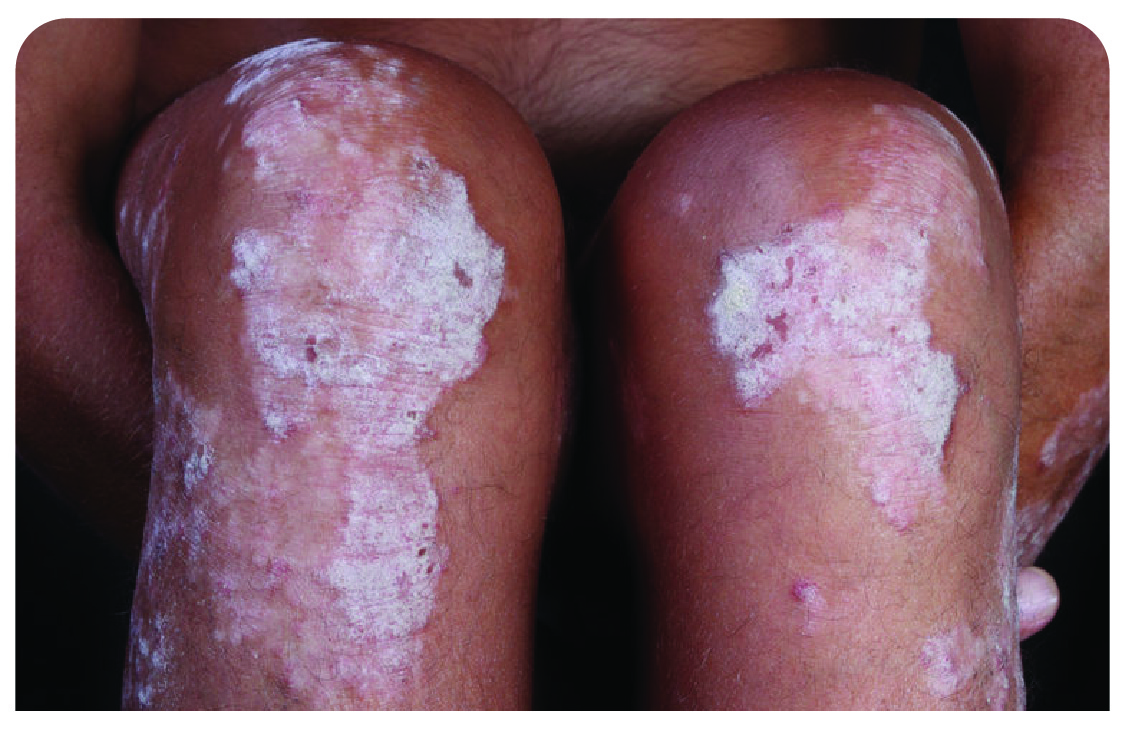
Begin with dry, red, and tender skin. Within hours, widespread pus-filled blisters can appear
Erythrodermic psoriasis
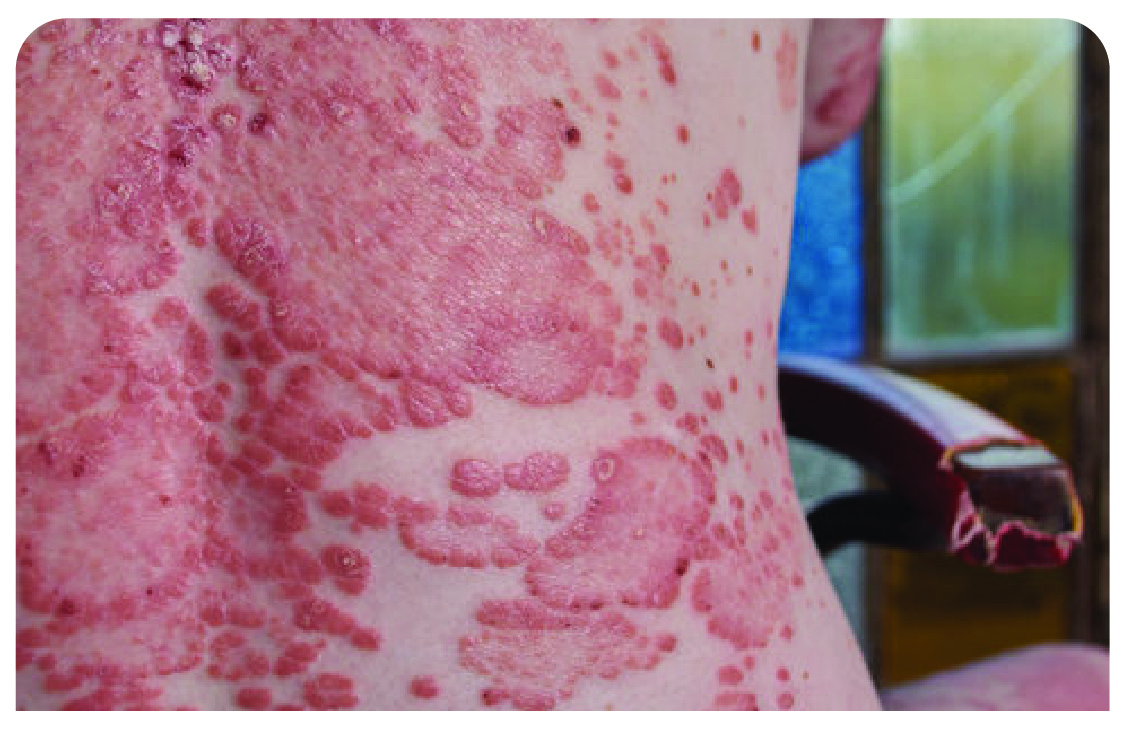
Large areas of skin can look as if burnt (the serious type which needs immediate medical attention)
What causes psoriasis?
No one knows the exact cause of psoriasis, but experts say that it’s a combination of many factors. If something is wrong with the immune system, it causes swelling, triggering new skin cells to form quickly.
Skin cells are normally replaced every 10 to 30 days; however, in psoriasis, they grow every 3 to 4 days.
The accumulation of old cells being replaced by new ones creates those silver scales.
SPOT THE SYMPTOMS
What are the signs and symptoms of psoriasis?
Dry, thick, and raised patches on the skin, often covered with a silvery-white coating called scale, that usually itches a lot. While thickened, dry skin patches are common; psoriasis can cause many other signs and symptoms.
What one sees and feels may tend to vary with:
- Type of psoriasis a person has
- Places where these spots of psoriasis appear on the body
- Amount of psoriasis present on the body
Psoriasis symptoms

Red patches on skin
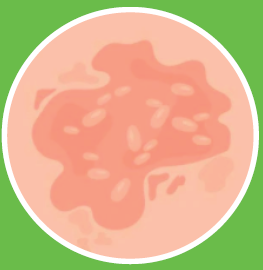
Small scaling spots
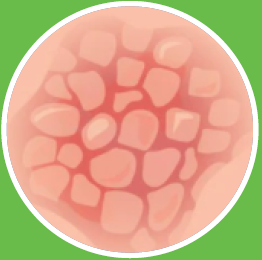
Cracked skin
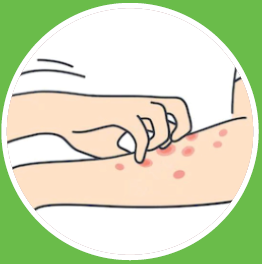
Itching
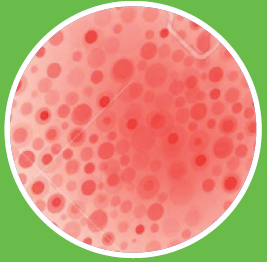
Soreness
Thickened nails
Swollen and stiff joints
WHAT CAN TRIGGER PSORIASIS?
Many routine and common things can act as triggers, resulting in psoriasis appearing for the first time.
What are the common triggers?

Stress
Skin injury like a cut or a bad sunburn

Throat or skin infections
Some medications

Cold and dry weather

Tobacco

Obesity

Excess sunlight

Heavy alcohol intake

Hormonal changes
Triggers can also cause psoriasis flare-ups. Triggers are different for different people. For instance, extreme stress may trigger psoriasis for someone, whereas cold weather can be a triggering factor for another.
Hence, it’s crucial for people with psoriasis to know what triggers their condition. If one can avoid these triggers, flare-ups can be automatically reduced.
If one suspects psoriasis, it’s important to seek medical help or consult a skin specialist. Treatment can help relieve the discomfort and give a clearer skin.
What happens when psoriasis is left untreated?
Untreated psoriasis can cause plaques to continue to build and spread, causing many physical and emotional complications.
These include-
Physical Complications
- Painful and severely itching plaques
- Infected plaques and scars
- Permanent hair loss in case of scalp psoriasis
- Painful and weak nails that can easily be detached from fingers
- Joint pain, stiffness, and swelling can gradually develop, causing psoriatic arthritis
Emotional Complications
HOW IS PSORIASIS MANAGED?
How does a doctor diagnose psoriasis?
A doctor can often diagnose psoriasis based on how the skin appears. They may be able to confirm whether a person has psoriasis or not, using the following approaches:
Doctor will look at and examine the skin and the affected areas
In rare cases, a small skin portion will be sent for examination
Doctor will ask questions related to the disease history in past, if anyone in the family has/had psoriasis etc.
A specialist in diagnosing and treating skin conditions is called a dermatologist. A dermatologist can examine the skin and help provide relief from the symptoms.
Should psoriasis be treated?
Treating psoriasis is good for both the body and mind. Treatment can:
WHAT ARE THE TREATMENT OPTIONS FOR PSORIASIS?
A doctor is the best person to suggest the most suitable treatment for psoriasis, whether it’s a family doctor or a specialist like a dermatologist. Major therapies available for people with psoriasis include-

Creams and lotions to be applied on the skin
Oral or injected Medications