WHAT SHOULD ONE KNOW ABOUT PSORIATIC ARTHRITIS?
Psoriatic arthritis (PsA) is a disease that can cause joint pain, stiffness and swelling. In most cases, PsA typically develops after the onset of psoriasis. But for some, the joint problems begin before skin patches appear or at the same time.

Swelling

Stiffness

Joint pain
How does psoriatic arthritis occur?
The body’s immune system acts as a defence against various harmful germs and bacteria. It protects the body from many infections and illnesses.
Sometimes, the immune system mistakenly attacks the body’s healthy cells. This causes damage to the healthy tissues of the body leading to auto-immune conditions. One such condition is PsA, where the abnormal immune response causes inflammation of the overproduction of skin cells. PsA can affect various joints. Refer to the image below for a better understanding.
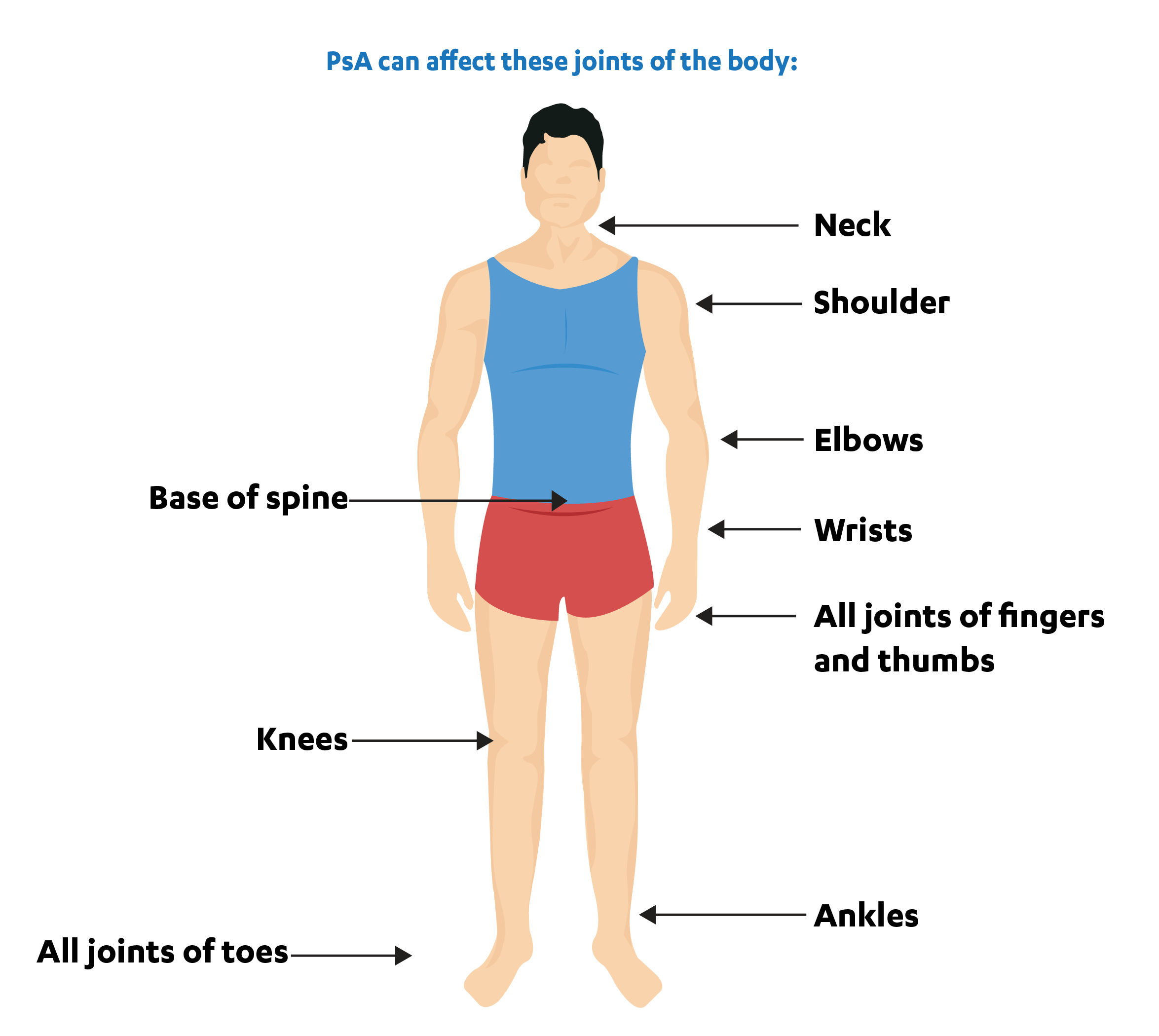
Who can get psoriatic arthritis?
Following factors can increase and affect the probability of a person getting PsA.
Having psoriasis

Family history

Aged between 30 and 50
LET’S UNDERSTAND THE TYPICAL SYMPTOMS OF PSORIATIC ARTHRITIS
PsA can affect joints on one or both sides of the body.
Symptoms can range from mild to severe.
Swollen fingers and toes
Along with swollen fingers and toes, joints get painful, puffy,and occasionally hot and red.
Stiff joints
Very common and may get worse in the morning.
Foot pain
Can occur especially at the back of the heels or sole of the foot.
Shoulder and back pain
Due to swelling, one could experience a pain in the neck, lower back, and buttocks.
What does a psoriatic arthritis flare-up and remission mean?
Flare-ups: Brief period when symptoms of PsA become worse.
Remission: The times when symptoms get better.
Note: A PsA flare can be hard to predict, but it is possible to reduce the frequency of flare-ups and minimize or prevent long-term damage to the joints with appropriate treatment.
Are there any triggers for psoriatic arthritis flare-ups?
PsA flare-ups are hard to predict. The nature and severity of flare-ups could differ from person to person. Actual triggers of a PsA flare-up in the body are mostly unclear and can vary widely and even change throughout a person’s life. Here are different triggers of PsA flare-ups:
Stress
Stress is one of the most common triggers for flare-ups as it causes swelling to surge. Also, stress and psoriasis are closely linked. Flare-ups are likely to happen when stressed, and psoriasis can increase stress levels
Injury or infections of skin or illness
Skin infections or injuries can cause aggravation or flare-ups at the site. Falling ill and overexertion can also result in flare-ups.
Not taking medication regularly
It is crucial to take medications as prescribed to prevent PsA from flaring up even if symptoms improve.
Unhealthy lifestyle
Smoking, eating fried or sugary foods and being overweight can cause PsA symptoms to worsen.
What happens when psoriatic arthritis is left untreated?
PsA may range from mild to severe. Regardless of the severity, it is important to seek treatment. If left untreated, PsA can cause permanent joint damage and disabilities. Furthermore, PsA can lead to various other complications if not treated early.
PsA can result in multiple complications like:
Decreased function and disability: Due to joint and tendon damage.
Eye problems: Like pink eyes (conjunctivitis) or uveitis. Such problems can cause pain, redness and blurred vision. Other complications include heart disease, obesity and depression.
HOW IS PSORIATIC ARTHRITIS MANAGED?
When to visit a doctor?
- See a doctor in case of persistent pain, swelling or stiffness in the joints – even if psoriasis is not present.
- Persons with psoriasis should get regular check-ups at least once a year to monitor their condition.
The doctor might carry out the following to arrive at the diagnosis
Physical examination:
A doctor will check the joints of a person for swelling, tenderness, and range of motion. Skin will also be checked for signs of psoriasis.
Blood tests:
To check for certain factors which are responsible for PsA.
Joint scan
To conduct a detailed examination of the joint structure.
How can treatment of psoriatic arthritis help?
The treatment for PsA can help:
What does the treatment include?
Below are a few treatment approaches for treating PsA. A doctor is the right person to choose the required treatment for a patient. Here are a few treatment approaches.

Initial lifestyle Changes
Right eating, exercise, and good sleeping habits may be beneficial.
Medications
Help in relieving pain, prevent or slow down joint damage, lower the disability and enable a person to live well.
Surgery
Based on the disease severity, a doctor may recommend surgery to reduce pain and fix deformities.




